[mashshare]
It’s amazing how important the feet are to an athlete’s health and well-being. And if you’re in the speed game, managing foot care is essential to athlete health. In this article, I cover the painful process of knowing what it takes to get results from sports podiatry, and I review details so you can succeed.
What Is a Sports Podiatrist?
A sports podiatrist is not only a foot doctor familiar with sports but also a highly trained specialist who understands the nuances of sport injuries and sports performance. A sports podiatrist is a clinical professional who is in the trenches solving problems and treating athletes. And some are involved in research.
Much of their work is limited to the foot and ankle, but on rare occasions they solve issues up the kinetic chain as high as the neck. Many sports podiatrists perform surgeries, some screen the foot, and others manage injuries by combining manual therapies and helping athletes get the right prescriptions.
Every time the foot hits the ground, a lot of force travels upstream through the bones and connective tissue. Good sports podiatrists help manage the forces properly by doing damage control; they don’t fix everything because they can’t resolve everything. That requires a group effort. Finding a great podiatrist who is local may not be possible, so expect to travel. And look for one who not only understands foot function but also total athlete health.
Below are services offered and the hard lessons I’ve learned when working with sports medicine teams. I also review the difficult realities of working with sports podiatrists. Although many great physical therapists overlap with the information covered here, a sports podiatrist is the best fit when the foot hits the ground.

Foot Assessments and Screening
If your podiatrist only glances at how your athlete’s heel and foot interact with the ground and pulls out a pen to prescribe an orthotic, run away. A comprehensive foot exam is a long process that requires a lot of quantification and testing—not just patient history. When it seems like the foot evaluation is taking too long and you want an immediate answer, instead of feeling annoyed be grateful. The biggest gripe in sports medicine is rushing to judgment instead of fact-finding. A good podiatrist usually has a private practice, which allows plenty of time to evaluate the problem.
A comprehensive foot exam requires a lot of quantification and testing—not just patient history, says @spikesonly. Share on XA comprehensive exam is a bit of an art and lacks a standardized process, so it’s important to understand the components of a great exam to evaluate whether it will be useful or just a rush job. Don’t use time as a sign of thoroughness, though; some exams are quick because there’s an organized process. Expect a lot of anatomical points of either objective measurement or subjective feel and assessment.
For example, a good evaluation will include simple measures like ankle dorsiflexion and the great toe’s range of motion while a test will look at the stability of the medial and lateral columns. Other assessments may include the equinus of the rear foot and the motion of joints that are evaluated less often. The more information, the better. Because foot anatomy is very complicated, a diagnosis requires significant investigation.
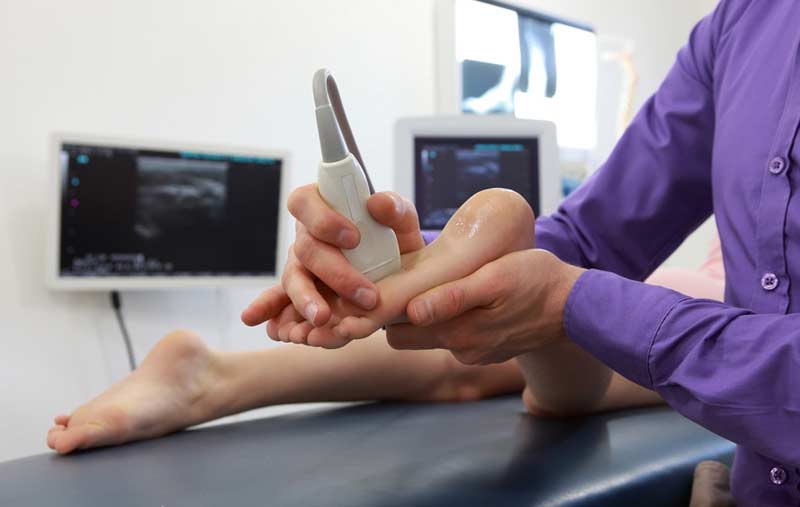
Additional testing, specifically imaging, is sometimes necessary. An x-ray, MRI, or sonography may be used to see how the structural area is trending as clinical symptoms are often misleading. It’s rare to look at imaging only and forego a clinical evaluation, although occasionally a problem is obvious and just needs confirmation.
Sometimes biomechanical testing—usually gait analysis—is used to fix an injury after rehabilitation, as injuries continue to show up or manifest in other areas if the underlying root problem isn’t solved. A great foot evaluation is only part of a complete evaluation, however, since footwear is also a part of the injury mechanism.

Shoe Evaluation
While athletes constantly receive misleading marketing messages, the hype around sneaker technology is in a class by itself. Companies make minor refinements look like magic pixie dust. Footwear, especially current technology, is either grossly overhyped or the advertising outright lies to the consumer. Some of the technology and designs are brilliant, but a great shoe may not jive with a specific foot. No footwear is right for everyone, so it’s important that your athlete brings all of the shoes they wear to compete, train, and walk around. It may sound extreme, but if they’re struggling with an injury, we do what we have to do.
A visual inspection starts with evaluating the wear of an athlete’s dress shoes or walking sneakers that are a little older. Elite sport shoes are tough to evaluate because athletes replace their footwear frequently—do a physical inspection as needed.
#PressureMapping shows how a foot interacts with a specific shoe anatomically and kinetically, says @spikesonly. Share on XEvaluating an athletic shoe or spike involves more than bending and feeling the shoe; we need to see how the foot interacts with it. Pressure mapping is commonly used to see how a foot interacts with a specific shoe anatomically and kinetically. We’ve discussed the technology twice on SimpliFaster (see pressure mapping buyer’s guide and identifying and treating high-pressure areas in the feet) and mentioned it a dozen times. I recommend checking out the guide on pressure mapping to become familiar with the technology.
Comfort is the first goal of footwear. A cleat that causes blisters or a high top that’s painful is not a great experience. Comfort is one thing and functional is another, so we need a balance between the two to help the foot use its anatomy. No sneaker, cleat, or spike is perfect.
Several good podiatrists review new models of popular brands every year, and many of them do it objectively using professional equipment. While this may sound extreme, ask the opinion of an NFL corner or defensive back who is out for the season because they had an Achilles rupture. The performance pursuits of new footwear sometimes compromise the risk and strain on the body, so we need to do our homework with all footwear changes. Even buying several pairs of the same shoe to create a stockpile can reveal small differences in manufacturing.

Orthotic Prescription and Testing
The NBA is a wild west for orthotics. It seems prescriptions are often based on foam boxes or plaster castings—this is Stone Age to me. And although an orthotic is sometimes considered a gimmick or crutch, I’ve seen more problems stem from inappropriate barefoot and minimalist training than from orthotics. If you don’t’ believe in wearing orthotics, take note—you may be wearing one and don’t know it. Some shoes are manufactured with added or removed material to create topography for the footwear.
I've seen more problems caused by inappropriate #barefoot and minimalist training than by orthotics, says @spikesonly. Share on XAny time you wear a modern sneaker, you must think about how this artificial device is interacting with your foot before pointing the finger at an orthotic. Orthotics are not for everyone, and a static device can do very little. New orthotics, however, using 3D printing and advanced engineering are changing their limitations. Regardless of the new technology, the foot is not much different than it was thousands of years ago, and an appliance can do only so much.
I’m suspicious of any orthotic prescribed for an athlete without pressure mapping. Over the counter options may provide a little comfort, but just handing a pair of polyurethane devices to an athlete qualifies as bad medicine. The combination of foot structure and function, running and sport mechanics, footwear, and surface interaction make orthotic prescription a tricky ordeal. Trusting an eyeball test or blind faith are also bad ideas.
If you don’t have pressure mapping, request a motion capture or similar evaluation. Finally, if these technologies are not available, do a treadmill video test for endurance and middle distance athletes. Sprinters and speed athletes need to be evaluated in the wild. Do a video analysis and bring the clips on a laptop or tablet with you to the appointment; it’s better than guessing.
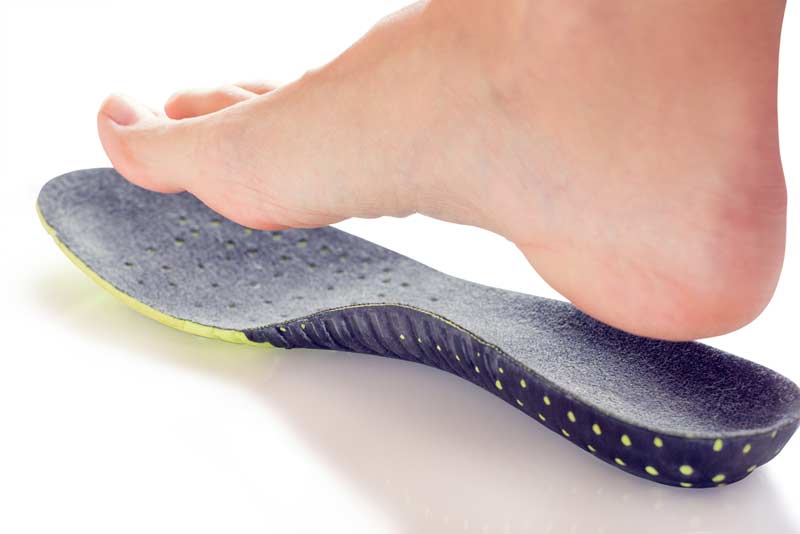
Sometimes orthotics are not necessary, and small modifiers like strips of hard felt-like materials can make enough changes that show up on electromyography or pressure mapping. When considering foot function, think about how many steps you take walking and running and multiply that by a thousand. Cumulative stress is a creeping danger, and often people recognize a problem when it’s too late.
Orthotics can contribute, but don’t expect them to solve life’s problems, as they are only part of the equation. While reducing load, preparing the body properly, and good coaching promote most of recovery, orthotics are often helpful. Also remember that bad anatomy and genetics are a reality, and we can’t do much except manage the anatomy and reduce expectations.

Training and Performance Consulting
Sports podiatrists are great for education as well. They’re often experts in biomechanics, though they’re not valued as much since they do more clinical work than research. My biggest gripe is that PhDs and DPMs are not working hand in hand often enough. Most of the research fails to look at foot screening and fails to become more granular with foot structure and function. Also, many podiatrists don’t know enough about the kinetic and kinematic aspects. Working with a podiatrist will give you an edge only if you hire the right one. Most sports podiatrists are not experts in performance, although this is changing.
The new breed of sports podiatrists is more biomechanically sound and does less general foot care, says @spikesonly. Share on XThe new breed of sports podiatrists is more biomechanically sound and they do less general foot care. A regular podiatrist has a higher range of requirements and does much more than treat athletes, so it’s hard for them to become familiar with the nuances of common soccer injuries due to poor cleat design when they’re also worried about diabetic ulcers.
On the other hand, having a wide range of experiences with regular foot needs does help, and these podiatrists are more skilled in knowing how simple issues can cause problems like ingrown toenails. The feet play an important role in athlete health and well-being, and simple things like wearing the right sandal can be a big deal if locker rooms are not clean (staph infections) or when a foot needs comfort instead of support after a big game.
A cool relationship exists with foot performance: a sharp rise in assisted output could increase risk while a drop in performance could lead to a big injury from inefficient force transmission. I wish more athletic footwear companies would work with podiatrists to see what happens when engineering becomes a little too aggressive. Biomechanics is great when it increases performance, but sometimes something has to give, and that could be a joint, tendon, or plantar fascia.

Rehabilitation and Injury Management
It’s great to work with a podiatrist during the return to play phase. They provide complementary care to assist the recovery of a lower extremity injury. Podiatrists should be part of the collaboration, as they’ve seen plenty of bad rehabilitation jobs fail.

I recommend having your athlete see a podiatrist early in an injury—not just a therapist or orthopedic specialist. Sports podiatrists specifically are good at evaluating which methods work after others fail. A great example is lateral ankle pains, where most of the return to play outcomes still include instability that’s observable and measurable.
Even if you don’t use a podiatrist directly in the return to play process, their initial comprehensive foot exam serves as the baseline return to. If something is still off, I would be very uncomfortable sending an athlete back to the field. Keep in mind that even baselines can be bad references because some athletes will struggle with lingering issues, which would make that baseline a poor goal. I don’t like using a baseline as a checkpoint to get back on the field; I just consider it the best option unless legacy tests are available. Tracking annual foot exams, gait testing, and even shoe selection are very useful for pinpointing potential problems.
Tracking annual foot exams, gait testing, and shoe selection help pinpoint potential problems, says @spikesonly. Share on XFinally, the best podiatrists are the ones who know when to let an athlete rest and not push things too quickly. Foot recovery is not fast and is very tricky, which is why boots and exoskeletons are growing in popularity again. Not being able to bear weight is a problem but too much stress can also cause problems. How many times do fifth metatarsal fractures fail to heal properly? It’s often not due to the surgery—it’s because the original problem was never fixed.
Seek out podiatrists to investigate problems forensically. You’ll be surprised how bad some rehabilitation programs are at understanding the etiology of injuries and instead are only good at reconditioning a problem.

Gait Analysis
A gait analysis includes a report; it’s not just watching an athlete running on a treadmill or track. Podiatrists watch for excessive or uncontrolled pronation, an extremely controversial issue in both clinical and research circles. When load management doesn’t work—meaning that training with the right amount of stress and rest fails to provide a good outcome—the culprit is pathomechanics.
Pain is not as important as function and performance because chronic pain may not be caused by actual damage, but ignoring pain is just foolish. Good sports podiatrists look at movement and help an athlete make changes that will contribute to success.

Arguments against treadmill testing focus on the difference between acceleration and running upright or maintain that a change of direction evaluation is needed to help with acute injuries such as ACL tears. True, a treadmill test is not perfect, but lab testing is super expensive and medical insurance rarely covers it.
A simple running test provides a lot of information, though. Even walking, which is not considered athletic, is the cornerstone to athlete health. While the foot strike may not represent sprinting as running tests do, it does highlight issues with joint function. Keep in mind most athletes who are severely injured can’t run, so baselines for both sports performance locomotion (running and cutting) and basic walking evaluation are good to have.
What should you expect from a gait analysis besides a technical summary of how you run and move? Not much if you don’t choose to commit to the recommended changes in technique or the interventions. Nothing’s guaranteed, though. Remember that mismanaging training load is the largest contributor to injury.
One of my concerns is asymmetry—it seems that because it exists so much, it’s considered normal. A bear attack, which is natural, offers a great example of something that’s not good for you. Asymmetry is not necessarily a problem, but it’s important to know the cause of asymmetry because many asymmetries lie on a threshold where fatigue or additional stress can lead to injury. Don’t be spooked by asymmetry, but don’t ignore it either.

Surgery and Minor Care
When surgery is necessary, you’ll have to decide if you want an orthopedic specialist or a podiatrist with advanced training. Small problems can often be taken care of by a podiatrist who understands how to do simple procedures. Other times you may need to go to a foot specialist who is an expert in complex surgeries. Podiatrists are excellent for non-surgical procedures that are minimally invasive. For example, small local injections of medications. Generally, you see a podiatrist so they’ll refer you out to a surgeon who will perform “human carpentry” of the foot and ankle.
You see a podiatrist so you don’t need to see a surgeon, as they intend to get you better without going under the knife. Most podiatrists understand the careful balance of getting back on the court, track, and practice field as soon as possible without risking further injury.
I recommend seeing a podiatrist like you see an eye doctor; you may have perfect “vision” now, but over time the feet age or could experience troubles. Extending the analogy further, look at the number of people who get Lasik surgery or eyeglasses if they don’t see well, but are skeptical after a podiatrist tries to correct a problem with orthotics. True, the analogy isn’t perfect, and outcomes with laser surgery that corrects the eyes isn’t a great example, but the argument does have merit. Rethink the podiatrist and remember they want to help and have dedicated their lives to making sure you get the care you need.
Final Recommendations on Sports Podiatrists
Look for a sports podiatrist who believes in conservative care. If you find one who is quick to recommend orthotics or surgery without giving rest and rehabilitation a try, get a second opinion pronto. Many podiatrists see athletes after years of failed treatment or care and witness damaged goods so broken even great expertise can’t save the patient from early retirement or surgery. It’s not fair to expect a podiatrist to solve injuries but they can add insight to reduce the strain on the foot and up the kinetic chain.
I recommend athletes see a podiatrist early in their career when they become a teenager. Regular checkups, even if the athlete is pain-free, are important, as it’s better to be proactive than reactive. Sports podiatrists are part of a winning sports medicine team, and I recommend looking for one now to better support your athletes.
Since you’re here…
…we have a small favor to ask. More people are reading SimpliFaster than ever, and each week we bring you compelling content from coaches, sport scientists, and physiotherapists who are devoted to building better athletes. Please take a moment to share the articles on social media, engage the authors with questions and comments below, and link to articles when appropriate if you have a blog or participate on forums of related topics. — SF
[mashshare]




