[mashshare]
Cryotherapy is one of my favorite topics in sports science and sports medicine, and I’ve monitored updates in the scientific research for a long time. After reading nearly 400 studies on thermotherapy and examining all of the variables, I’ve found using ice is still an enigma. Some new research, as well as some old conflicting research, still leaves the community with more questions about its value for sport.
It’s now in favor to abandon a lot of the old treatments, but before we scoff at using therapeutic cold, let’s scrutinize the research more. If you think ice baths are old news and cryosaunas are a waste of time, guess again. New perspectives about how the body recovers from injury and training reopen the door to cryotherapy.
Is Cryotherapy a Dead Practice Today?
Based on current vibes and practices in the mainstream arena, ice is considered either extinct or the primary way to treat injuries. Ask the majority of average Joes what to do after an injury, icing is likely the response. If you ask a sport scientist or performance coach whether to use an ice bath after hard training, those who’ve kept up with the current research will likely agree it has very little merit. Some noted opponents of ice therapy have written books against its use and devoted podcasts to promote its removal from recovery practices.
Yet we still see a lot of people swearing by cold’s value in sports medicine and sports recovery. A recent study found that cryotherapy increased mitochondrial changes, which is why some coaches still believe ice has value outside of pain management. While some see ice treatments going the way of VHS and cassette tapes—obsolescence—cold treatments aren’t going anywhere soon because they have benefits.
#Cryotherapy is alive and well because it helps manage athletes' pain, says @spikesonly. Share on XCryotherapy is alive and well because it helps manage athletes’ pain. It’s hard to say when heavy training enters the realm of injury, but the gray area is very difficult to navigate. Many athletes have to manage a continual state of soreness and microtrauma, and they look for a way to cope. For most people, including athletes, jumping into a tub of icy water is unpleasant, but when you’re looking for a way to escape unbearable soreness, it offers hope. Injuries, burnout, overtraining, fatigue, and chronic pain are still problems in modern sport. And until the root issues are solved, masking pain with topical approaches such as cryotherapy will not go away.
Here’s the key takeaway about cryotherapy: context and purpose are everything, like any modality. Chronically using cold water immersion (CWI) could decrease performance over time. But when considering world-class performance, the research may not represent what’s happening with elite athletes. When dealing with an acute injury, pain management may be worthwhile for those who can’t take medications. Each situation is unique, and declaring that ice is a dead practice is far from the truth, especially with emergency medicine.
In all honesty, the science does illustrate it’s not a great mainstream solution for supporting the body. Before we bury the ice bag or replace the tubs with blood flow restriction devices and tart cherry smoothies, let’s dive back into the science with a new set of eyes to set the record straight.
The Science of Cold Therapy
Cold generally decreases an organism’s metabolic activity while heat speeds it up. If we want to increase the healing of an injury or body, why would we slow it down? Most people simply look to the classic RICE model to treat injuries and to medical solutions to hasten recovery from non-medical needs such as training. And many sports medicine modalities have been reinvented as solutions for training recovery.
Chronic cold immersion may mitigate training adaptions, says @spikesonly. Share on XBut there’s a big difference between normal training symptoms and true medical trauma, as seen in animal studies. We do know that some sports medicine interventions simply don’t transfer to sports training, and repurposed methods and other solutions from injury models don’t have much to offer for training needs. In fact, some sports medicine methods, such as chronic immersion to cold, may dampen training adaptations and make things worse than doing nothing at all.
Cold therapy will not help reload glycogen stores nor regrow a torn tendon, obviously. But when we come to perceptions of fatigue—and not muscle cells or joint physiology—it seems a trade-off exists. Do we want the athlete to feel better or get better?
Much of the research with cryotherapy suggests it’s a placebo. If so, why do non-physiological placebos work just as well? In research, it’s very difficult to blind subjects and truly separate controls from the treatment intervention. We do know research has investigated four outcome measures and, for the most part, results from cryotherapy are not overwhelming.
Here are the four primary theoretical benefits to cold therapy:
- Pain—Theoretically, ice can target a nerve pathway and decrease pain when used sparingly. Ice may be an alternative to over the counter or prescription medications, but pain is very individual and should be managed by sports medicine.
- Soreness—For delayed onset muscle soreness (DOMS), cryotherapy can help in some cases when the athlete responds to this method. Training soreness—like dull aching in the legs or total body—tends to be more systemic and is accepted as normal as opposed to soreness in a specific part of the body like a treated Achilles tendon that might be injured.
- Swelling—So far research doesn’t support the notion that cryotherapy effectively helps with joint and muscle swelling; even the research on direct compression is mixed. Some research supports this, but it’s a coin flip whether it will work or not. Secondary injury is under scrutiny, and reducing the incidence of swelling in the first place is a nice strategy.
- Fatigue—During tournaments and other dense periods of competition, perceptual recovery and perhaps muscle oxygenation respond well to cold therapies such as CWI, according to some research.
These benefits are why athletes use cold, and I’m not sure what else cold could theoretically help with. Most of the research covers treating injury acutely with topical cooling (ice) and chronic and acute recovery with CWI. Other than the four potential benefits listed, cryotherapy doesn’t seem to be the modality of choice. Research has explored combined therapies, such as contrast heat and cold, but most of the studies investigate a single purpose and single modality.
The science of cold therapy is wide, simply because cold provides a continuum and that usually means how long and how cold. Spraying an athlete with vapocoolant is hardly the same as decreasing a person’s core temperature therapeutically to help save them after they just died from a cardiac arrest in an ambulance. What happens to the body locally, say with muscle tissue and tendons, isn’t the same as what happens with the autonomic nervous system and brain cells.
Examine the research and experiment to know if cold treatment works in your situation, says @spikesonly. Share on XIn addition to physiological responses, the feeling of body cooling while in hot environments or after a long flight is radically different from what happens immediately after practice. Precise factors like timing and sequence could make a therapy that’s found to be an impairment in the scientific literature a true advantage when used differently. Reading the exact details of the studies and experimenting with treatments are the only ways to know if a treatment can work in your situation.
Cold Water Immersion: Modulate the Autonomic System
The most common use of CWI is dunking an athlete to manage dead legs from a severe amount of training. I have very mixed feelings regarding the use of cold to mask an athlete’s agony after overload, which usually occurs during preseason practices.
During the preseason, a rush to get a team into form is the constant theme in elite sport. There’s not enough time to train, so coaches perform doubles and triples to get the work in, and strength coaches drop the weight room work and become the equivalent of get-back coaches for managing ice baths “workouts.” Knowing the athletes are overloaded and broken down, they’re smart enough to cease the strength training and focus on anything they think will help athletes cope with the extreme volumes and intensities.
If the athletes make it out of the pre-season, strength coaches ramp up weight training again. For the most part, though, they’re “recovery coaches” during a time they should be doing the opposite. During the general preparation phase (GPP) and specific preparation phase (SPP), athletes should be building up natural internal capacity and saving therapies for playoffs or peaking. Instead, coaches just do what they can and hope for the best. We need to do better collectively.

We do know that cold potentially sends the wrong cell signals. Over time this adds up, or more accurately subtracts from the intended strength gains. I’ve never liked the idea of intentionally using ice as part of training, viewing it as a bailout. In the research, immediately using cold after training decreased needed activity by the satellite cells in muscle fibers, and the strength adaptations were less than those who did nothing at all (control).
There are many variables to think about with CWI, including temperature, timing, depth, duration, and even the sequence of training. Logically, hopping in the tub immediately after training makes sense, since athletes are conveniently at the facility and are so sore they want something to cure their ailments. In my experience, however, if you need an artificial external solution repeatedly, you’re gambling and eventually will lose.
For a good alternative, look at the studies by Martin Buchheit and others, and time the therapy so it’s far enough apart from the stimuli, say 24 hours. By then most of the pathways have been in motion, so you can use a higher temperature than the typical protocols, which won’t interfere with the natural cascading biochemical reactions.
A cool bath—not icy or cold—is enough to feel soothing and refreshing without blunting the signal pathways. With careful timing, correct protocols, and shrewd management of the loading sequence, an athlete can receive the recovery benefits without losing the gains they need from their conditioning and strength sessions. If soreness is manageable, wait a day or two to help reduce adaptation impairment.
A cool bath 24 hours after training helps soothe & refresh without blunting nerve signal pathways, says @spikesonly. Share on XI’ve used a cold shock treatment for athletes who can take time off from intense training and competition, for example when they had an ankle sprain. It’s helped athletes get sleep when medications were inappropriate due to health risks or personal beliefs. Many athletes are hurt and over-trained at the same time, and one ice bath may be enough to get them out of their slump physiologically and psychologically. CWI may be appropriate a few choice times a year if it leads to a predicted measurable outcome. Otherwise it’s nothing more than superstition.
Topical Ice Treatment: Limited Support with Pain and Swelling
The connection between ice and injury has a long history, but the research on its value shrinks every year. One proponent against ice is Gary Reinl, who recently published a short book about how ice is an illusionary treatment. While his summary was meant to redirect the reader to electrostimulation for lymphatic drainage, it was totally fair about ice treatments.
And though I love electrical muscle stimulation (EMS) for passive recovery when travel and fatigue are high, hydrostatic pressure and actual movement provide far more lymphatic mobility than stimulating a leg with a stim-unit. Still, I would rather use EMS for post-injury treatment than toss an athlete a bag of ice, and I wish Gary explored pain management more. While he did discuss NSAIDs (nonsteroidal anti-inflammatories), he focused on the swelling and inflammation argument, not a true repair model that we need.
The lymphatic system is not completely passive; the research describes it as a combination of active and passive contractions that helps move materials throughout the body. When an athlete injuries their body or experiences severe eccentric damage, the surrounding fluid swells around the damaged area. The question is: does secondary injury occur from the swelling, and does removing the swelling speed up the healing process or does it only provide comfort.
Cold therapy is not an impressive way to reducing swelling, says @spikesonly. Share on XBased on post-surgical experiences and watching the changes that followed various cryotherapy approaches, I’ve found cold therapy is not an impressive way to reducing swelling. Damaged tissue needs a healthy environment, and cold does not foster growth in the neuromuscular system.
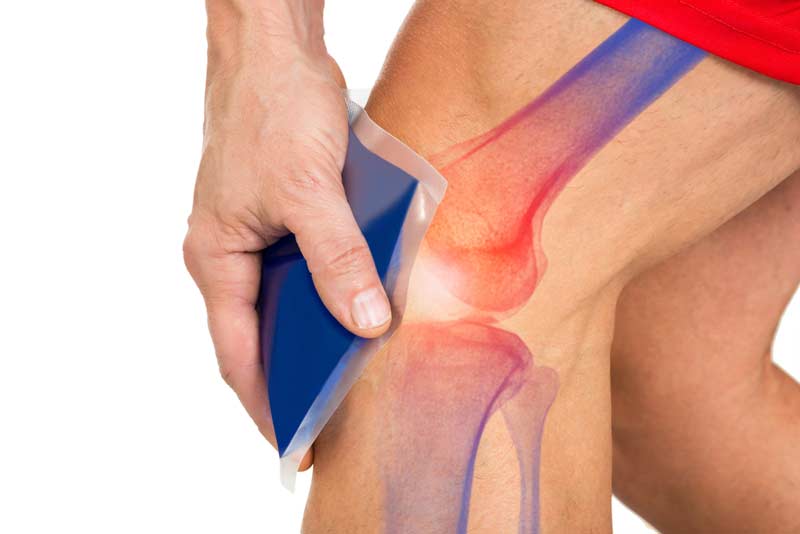
Pain is a very different story than swelling. While they’re both connected to injury, an injury may not cause pain. We know pain is modulated by cooling due to research studies, which demonstrated that a decrease in tissue temperature causes a physiological response to the nerve when done well. Cooling the nerve changes the conduction speed and may alleviate some discomfort from injury or soreness from excessive training.
Contrast Showers and Other Modalities
Contrast therapy is a classic approach to recovery by either repeating alternating short periods of cold and hot or having an extended period at one temperature and then switching to the opposite temperature. Based on the research, there’s no evidence that contrast therapy improves healing.
There is some intriguing research that shows cold showers and other methods may be valuable for low-level depression. Contrast showers and contrast immersion therapy don’t seem to have a physiological benefit, but the authors concluded they could provide a psychological advantage. In my opinion, this may work with deep overtraining. But it’s lazy to use it as a dash of salt for good luck.

One study of pain treatment after surgery compared continuous cryotherapy to conventional ice treatments and found that the difference wasn’t exciting enough to show value, but the authors did discuss its convenience as an advantage. So, when investing in cryotherapy, a simple budgeting plan must be in place to track how money is spent and what you’re truly paying for. Pre-cooling strategies may have a place in addition to post-treatment, including slush beverages.
Water therapy’s benefits are clear when the sessions are active, and passive hydrotherapy can make a difference in training camps. One study performed a while ago found water therapy with a warm water jet spray on the muscles while submerged helped athletes recover between heavy sessions. Outside of that training camp study, there’s not much evidence available to demonstrate the value of immersion modalities regardless of temperature.
Cold followed by heat has a positive mental impact on wellness indicators and #HRV, says @spikesonly. Share on XI’m a firm believer that cold therapy followed by heat later feels great, and plenty of athletes have found the cold to warm or even hot sequence is a great spa experience during times when training and competition are overwhelming. There are no changes in jump performance or recovery times, but mentally the changes were noticeable in HRV and other wellness indicators. The brain is still an uncharted area in science—we do know the grind is a little easier with comfort food and a session of “feel good” time.
Before You Head Back to the Ice Age
You can’t play around with cold. There are real issues with frostbite and risk of serious complications if you don’t do your due diligence. Cryotherapy provides a complementary solution that’s not necessary, but it is likely helpful. Knowing the science and the practical applications of ice and cold therapy can more effectively help elite athletes and those who manage sports medicine challenges. We know that ice is not a magic bullet as once believed, but it’s also not a bane to healing.
Since you’re here…
…we have a small favor to ask. More people are reading SimpliFaster than ever, and each week we bring you compelling content from coaches, sport scientists, and physiotherapists who are devoted to building better athletes. Please take a moment to share the articles on social media, engage the authors with questions and comments below, and link to articles when appropriate if you have a blog or participate on forums of related topics. — SF
[mashshare]




