[mashshare]

I’m new to anterior cruciate ligament (ACL) rehabilitation and have learned a lot over the last few months while working with some very smart physical therapists and athletic trainers. Although I’ve never had an athlete tear an ACL while under my care, I have had athletes come to work with me with previous ACL injuries. Many of them had botched rehab jobs, but some were rehabilitated amazingly well. Unfortunately I’ve also observed lazy professionals go through the motions.
The human knee is a complex system, even if it’s considered just a hinge joint to anatomists. If you are new to ACL rehabilitation, you’ll find a wealth of information in this article. If you’re a therapist with decades of experience, I promise you’ll find nuggets of wisdom that you’ll find valuable. Even if you don’t rehab athletes, these ideas and concepts will be worth your time to read.
A Word of Caution Before You Start
The information below covers the entire time continuum of ACL rehabilitation, meaning it doesn’t matter if your athletes come to you right after surgery or at the end of their return to play. If you’re working with the athlete from start to finish, obviously all of the concepts will help. Many coaches are jumping into ACL return to play programs more and more.
I suggest exercising caution early, as some coaches get overzealous with loading. More strength coaches are getting involved in this process because rehabilitation is training, just with a specific limitation. Medical professionals are needed to handle the post-surgical period to ensure everything heals smoothly. Use the concepts wisely and adjust accordingly for your athlete’s needs and situation.

Start With the Brain but Don’t Forget the Soul
The best truth serum for the athlete’s inner self can be a major injury like an ACL tear. Although the current trend seems to focus on the brain, the entire human experience is more important. While the soul is not something you can put under the microscope, it’s something you must manage person to person, not from device to human. Neurologically, an injury requires central nervous system (CNS) involvement, and it will take months and perhaps years to re-educate the body. While the scars of surgery may fade, the emotional scars can be the real challenge to healing.

A secret luxury exists in a team sport: physical performance is never maximized because of the needs and requirements for tactical and technical skills. An athlete who is not fully maximized has room for growth, a perspective that provides hope for a wounded player who needs something to believe in. I have seen Olympic athletes in time-for-place events come back from ACL tears and win medals; even sports that are more absolute have a little room for improvement.
I use a polarized approach to rehab severe injuries. I know the athlete needs both social and emotional group support as well as the private technical attention of working one-on-one. Even today, I’m shocked by how much sports psychology is involved with healthy athletes, never mind injured ones.
Athletes will often feel isolated when training on their own and believe they’re falling behind. To help prevent this, I give team sport athletes opportunities to work with Olympic sport athletes. This gives them a mental edge and helps them feel they’re part of something. It’s not easy to juggle different stages of rehab or training, but it works.
Conversely, when we do the specific one-on-one training work, we can zoom into uncharted waters of fears and emotions that sometimes get channeled out in a private environment. I suggest focusing on the balance of both elements, and program these athletes with more attention, nearly double the efforts and attention than before their injury. It will pay off.

Use Electrical Muscle Stimulation Early and Correctly
I have written three articles on Electrical Muscle Stimulation (EMS) for SimpliFaster, discussing the science of electrostimulation, the protocols for performance, and the recovery from travel. I still see EMS overlooked and considered something that’s added for the sake of a checklist instead of a training focal point.
Athletes must buy into #EMS and understand its goals. Coaches need to understand its value, says @spikesonly. Share on XWhen the body is cut, even arthroscopically, the rules to the game reset and are far harder with athletes now than ever. Acting complacent and tacking on electrodes is lazy. Athletes must buy into EMS and understand its goals. While I believe any methodology will distill to a protocol, EMS requires more than “sets and reps” with its application. EMS concerns the feedback and connection between an athlete and the environment–the hardware does not do the work for you.
Functional EMS, and trust during activities involving stance, are concepts I learned this year. An athlete will believe that their injured or repaired leg is weaker than it was, and just looking at a slightly atrophied muscle will evoke insecurity in the joint. EMS solves this problem by telling the athlete that we’ve prepared for this situation, and we already know what to do. Creating a very small amount of success peripherally helps create freedom for the athlete to build their neurological circuit centrally. Any exercise superimposed with EMS should not be considered a crutch option, but considered a way to tell the athlete “no excuses.”
Recently Damian Harper tweeted about an EMS and Eccentric training protocol and, at first, I was disappointed that EMS was not effective. But the study didn’t combine the model simultaneously. In the EMS protocol, the researchers split the period of exposure equally between eccentric training and only EMS.
#EMS alone will never create the necessary strength or function needed to return to play, says @spikesonly. Share on XEMS alone will never create the necessary strength or function needed to return to play. Coaches need to realize that, although EMS is a small part of the equation, its value is high enough to include in a program because it provides a great framework for feedback that therapists can tap into.

Train Hard Everywhere Else–Within Reason
I have a saying for athletes, “Losers rehab, winners reload.” It’s very true and fires up an athlete who needs to believe in something. That simple four-word phrase is powerful because it tells the athlete that you’ve been there before, and you have a higher standard.
During the rehabilitation process, we need to tell some athletes that they simply didn’t prepare well. Not all injured athletes should be faulted for injury, but many athletes who do get hurt from laziness and unfocused training are often coddled and foolishly treated like victims because they’re talented or popular. Some athletes may never learn to connect hard work to being injury-free, but when one ends up in the garage with an injury, it’s a blessing in disguise if they’re treated appropriately.
Many coaches, myself included, realize that one small tiny fraction of the body, say 1%, shouldn’t allow an athlete to become a couch potato. When life gives us lemons, it’s tempting to make lemonade by the gallons. But training too hard around an injury is an overreaction.
In the past, I used to get overly excited to use an injured athlete’s down time to make them better. While most of the time it worked, a few times I realized if I’d gone just a tad easier, the injury would have healed deeper; we focused too many biological resources on training rather than healing the injury. My mistake wasn’t a big one, but it was enough for me to feel the difference when I rectified it.
Harmonize healing and training and monitor physiological status when planning return to play, says @spikesonly. Share on XHealing and training in harmony make a great plan for a return to play. And monitoring an athlete’s physiological status is instrumental to knowing how many days of strain and recovery occur in a period of time. My article on HRV monitoring should have included more on rehabilitation because having an indication of the body’s entire state can safeguard against going a little too hard. While I don’t have a perfect scoring system because the science is too complex for a chart or formula, an excellent rule of thumb is to see the direction of the rolling average and adjust accordingly. It’s not fancy or exciting, but a trend is a direction, and athletes need it to go up.

Use Running Mechanics to Screen, Use Cutting to Train
Human locomotion, or gait, is the cornerstone of all movement. We take it for granted until we lose it. Many ACL tests are too ligament-centric and do a poor job of evaluating movements other than hop and stop. I’ve learned that coaching running is a great test for motor learning for athletes who tear their knees. When I get brought in, I used to figure my role was to bring back an athlete’s speed or to work on technique. I now understand my job is to expose them to learning outside of a tactic on the field or skill with a ball.
Track coaches employ drills to teach movements, and some of the smart therapists like drills because they create a learning template for injured athletes. As mentioned earlier, drills may not teach an athlete to sprint faster, but they may help wring out the sponge, so they learn to acquire better form when they do sprint. The specific Bosch exercises may not be the solution for ACL rehab, but the principles behind some of them have merit.
Cutting, #deceleration are prime culprits for causing injury, so they’re the perfect antidote, says @spikesonly. Share on XCutting and deceleration are prime culprits for causing injury, and this makes them the perfect antidote. Too many times I see coaches who want to choreograph technique, thinking deceleration mechanics were the problem. If this were true, ACL injuries would be like UCL injuries which break down over time. Instead, ACL injuries happen acutely.
I’m all for technique, but I argue that reflexive and reactive skills require more training demand because fast and unexpected movements need high rates of force development and eccentric strength. I train agility generally with more overload, and train sprinting more specifically with direct options. Connecting general and specific work with instruction is important. No matter how well you can coach, however, you can’t teach something to the brain that requires a quality of strength that athletes don’t have. Eventually you have to train with overload principles.
The plyometrics training inventory along with comprehensive lower body strength training is not new to coaches; what’s new are ways to evaluate their transfer. Here is a quick list of exercises and respective evaluation scoring ideas that I’ve learned.
Rotational Hops–Lateral hops and projection plyometrics are great and are enough to make a lot of progress. Since game demands require dimensional abilities, it makes sense to include rotational work in the final stages. Coaches should evaluate the entire body’s quality of movement, as well as the speed and range athletes can manage with skill.
Contact Jumps–Pushing athletes in different directions while in mid-air is popular, but simply randomizing directions won’t prepare for sport. Use other variables, for example no contact at all, and follow-up movements that expand the demand beyond bracing for impact. Evaluate based on speed and transitional technique.
Eccentric Lateral Lunges–Lunges with rapid drops and eccentric spikes are excellent options to keep athletes sharp for general cutting abilities. I don’t do any Heiden work until an athlete can do lateral lunges, and sometimes it’s necessary to regress with lateral squats. For most field sports, I like to work up to an eccentric load 120% of body weight.
Reactive Field Work–Reaction agility before ball work makes sense. As soon as the athlete runs and decelerates well, they tend to jump right into ball training. This is where the problems start again. Adding reactive agility will not make the next Ronaldo or Iverson, but it will prepare athletes for the rigors of their sport better than not including it at all.
More exercises and options exist of course, but the point is to make sure each stage has criteria for success before moving on. Nothing is a perfect linear model, but most coaches get into trouble by overthinking and not appreciating simple loading progressions. When in doubt, make it clear and simple, and progress incrementally.

Improve Your Jumps Force Analysis
Matt Jordan presented his findings regarding symmetry and ACL tears at the NSCA Conference in May. His information was right on the money–doing only a countermovement jump is not enough to determine function. This reminded me of another conference seven years earlier when we watched a video of Cam Newton rehabbing a knee. Interestingly, the injured leg outperformed the healthy knee kinematically in the single leg hops.
We currently see a lot of opinions on force plate readings based on beliefs rather than good science. If we look at the research, asymmetry is normal at times, but a change in asymmetry due to poor function is not acceptable.
Vertical jump tests not only evaluate height or peak force, but also an array of coordinative expressions of proprioception, power, and joint function. Therefore, a battery of tests with multiple scoring parameters is better than one test in isolation. Repeatedly rehearsing one test will not reveal more information, just small changes over time.
The tests that matter to me are single leg hops and an appropriate reactivity test. These two deserve inclusion in the commonly performed Bosco tests. Here are two metrics that may help provide the right information to those on the return to play team. While I’ve learned these recently, I’ve instinctually known that they have value for more than just the performance of healthy athletes.
Stiffness Index–It’s important to look at the RSI both bilaterally and individually for jumps and hops. When jumping with two legs, athletes can mask injuries and compensate with amazing strategies. Isolating individual legs exposes injuries.
Eccentric RFD–Specifically measuring RFD (Rate of Force Development) a bit cloudy. RFD is hard to evaluate because it’s challenging to define when the intent begins. With countermovement jumps, we can calculate eccentric RFD, and I’m a fan of both the average and individual right and left measures.
Of course more tests exist, but I like the stiffness measures in the early strength phase because it exposes how athletes compensate. Seeing how an athlete brakes eccentrically with force plates is enlightening, but coaches must be firm on the protocol so they keep the movement patterns similar for comparison.

Have a Skilled Sport Podiatrist Evaluate the Foot
There are many reasons for ACL tears in sport. Eccentric strength, proprioception, mechanics, and fatigue are all part of the equation. As is foot function. Strangely we see a proximal obsession with core training and very little attention to the joint system below the ankle. I expressed my concern in my article about training the core; if the torso and pelvis are part of the spinal engine, having bad tires (poor foot function) prevents having a winning formula.
I have athletes fly to Chicago because we don’t have many skilled podiatrists who know enough about sports in my area. Many are great for a simple assessment, but if I need to solve a problem pronto, we hop on a plane to the Windy City. I’ve used Bruce Williams for seven years, and each time I learn more about the connections between the foot and ACL. I also learn how hard his job is.
Strength coaches are responsible for strengthening the muscles that support the knee, and they’re also responsible for knowing when to refer out. I believe that referring out is scary for some professionals who don’t want to let go of control or who believe it adds work that doesn’t seem worth the effort. Regardless, barefoot training isn’t solving every problem, and the research shows it’s limited and sometimes dangerous–for example, with minimal shoe running.
Some athletes have normal pronation patterns regarding range. High velocity coupled with other restrictions can lead to valgus issues during cutting maneuvers or rapid deceleration. Add fatigue and long seasons, and athletes continue to tear ACLs. This trend is not going away.
In the NFL, about half the injuries occur during the short preseason, about 25 tears. Just under 50 ACL tears per year happen in the NFL, and this won’t be solved by monitoring athletes and prescribing eccentric training alone. I don’t have the expertise to give this section justice to explain the connections between such a complex joint system as the foot and the mechanism of tearing the ACL from non-contact.
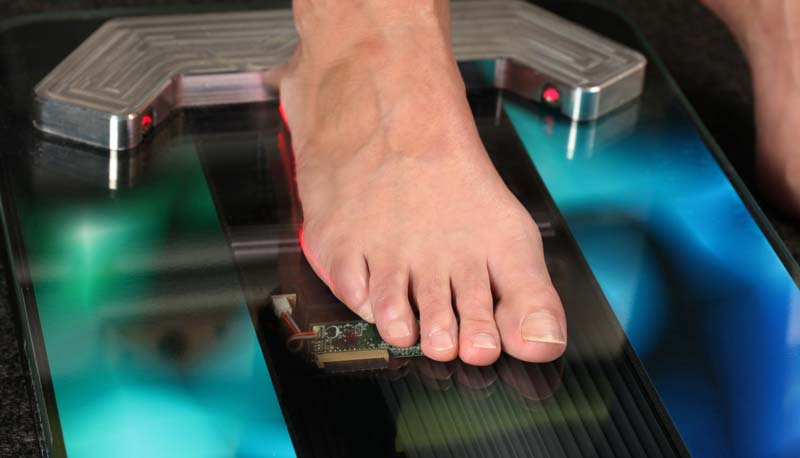
Pressure mapping & clinical evaluation of the foot are essential to mitigate the risk of #ACL tears, says @spikesonly. Share on XI do have enough experience to see how pressure mapping and clinical evaluation is essential to mitigate the risk. Every athlete that plays on their feet should get screened and evaluated. Nothing is surefire, but proper footwear and management of foot mechanics give an athlete a better chance for success.

Use Precision with Biofeedback Plyometrics
Electronic timing and Velocity Based Training provide instantaneous feedback in training sessions, but plyometrics seem to be limited to the height of a hurdle or box. Sometimes coaches will measure distance. But in the world of biofeedback, the result of a performance and the measures that make up a performance are vastly different. Video feedback is excellent, but the fusion of kinetic and kinematic data is a game changer.
When training plyometrics for ACL rehabilitation, it’s essential to give instant objective information directly to the athlete. Remember, after an athlete has surgery to repair an injury, their nervous system still needs calibration; biofeedback accelerates the process and improves the outcomes better when compared to not using it. Technology is never a replacement for coaching or medical support, but it does weaponize the process.
When maximal outputs are not an option for rehabilitation, it’s easy for an athlete to get caught up in the fact that their power and force capabilities are not the same. Competitive athletes want to be as fast and explosive as they were before their injury, and early-level plyometrics can feel humiliating when they’re used to performing feats of greatness. Ironically most talented and powerful athletes may lack foundational skills at lower level exercises.
As mentioned earlier, athletes also need to know they’re training as they did in the past, so it’s fine to push the non-injured leg within reason. Biofeedback keeps the process in check. While it’s tempting to chase PRs in the weight room to feed an athlete’s ego, the goal is to give the athlete enough hope to be positive, not spoiled by fantasy numbers.
Biofeedback doesn’t need to be complicated. A 5-second delay and a smartphone connected to a flat screen is a great start. Coaches can add EMG and focus on very simple, nearly binary, responses with muscle activation. Other ideas are more quantified, like focusing on rhythm and symmetry, two qualities that don’t discourage athletes as much as absolute legacy measures do. They key to biofeedback is development and providing direct objective information the athlete can trust.
Biofeedback also removes the possible friction between the athlete and the coach or therapist because the data is directly in front of them; the one doing the rehab with the athlete is not the bearer of bad news. Any time a technology can connect an athlete and a professional, it’s a win.

Progress Chaos Slowly and Systematically
Some ideas about movement variability have been so blown out of proportion that coaches think that junk repetitions of random noise will somehow build resilient athletes. True, a wide range of mechanical loading angles and speeds help an athlete become accustomed to possible playing situations, but the bastardization of this concept has done more harm than good. Anytime a “new” concept is shared at a weekend conference, the following Monday becomes a social media highlight series of silly exercises that make me cringe. Chaos is a cool term, controlled chaos is a sexier term, but progression is what separates mindless variations into a system with checks and balances.

I’m not a huge fan of injecting chaos into an equation that usually has enough of it already, but do plan some progressions that will prepare an athlete for the demands of the sport. It’s true that sometimes unexpected things happen, but the likelihood of a goaltender needing to run multiple 100m sprints back to back to back is like doing financial planning before playing Powerball. The constraints of a modern game mean we know the possibility of what could happen, and being a betting man, I always prepare for what is probable or likely.
Chaos or excessive movement variability early is too much too soon after surgery. During ACL training, getting an athlete to walk is enough of a challenge, adding excessive balance or instability is just delaying success when real preparation is needed.
Progressions of chaos follow the same training rules as progressions of training. The rules of progressions require us to judge what the athlete does successfully and what incremental steps are logical to advance the athlete. Adding chaos is not an excuse to let anything go in training, it’s just an element of variation that challenges the athlete with a wider pool of stimuli.
Improve ACL Return to Play with Confidence
I feel strongly about the success rate of my work because we had very solid evidence that what we did was working. I’m not saying that if you don’t have data, you can’t justify your training and rehab. In this day and age, however, not measuring is negligent if you’re in high-level sport. Most of the concepts above are timeless; they’re not new. The new wrinkle is that adding the right technology or the right methodology is enough to advance a program to achieve better results.
I learned so much this past year and know that, after a few more seasons of being part of a talented team, I will be competent to handle athletes without second guessing myself.
Since you’re here…
…we have a small favor to ask. More people are reading SimpliFaster than ever, and each week we bring you compelling content from coaches, sport scientists, and physiotherapists who are devoted to building better athletes. Please take a moment to share the articles on social media, engage the authors with questions and comments below, and link to articles when appropriate if you have a blog or participate on forums of related topics. — SF
[mashshare]




