[mashshare]
Nothing scares coaches and athletes more than Achilles injuries. They are difficult to manage, and traumatic injuries ruin many careers. Sometimes an athlete will only experience a little soreness while other times the pain from a rupture is so debilitating that people pass out. Achilles tendinopathy research seemed to stagnate during the last few years, but a few great studies have surfaced that may lead us out of the medical dark age in sports.
For athletes, coaches, and sports medicine professionals, this article will share relevant risk factors. It’s not a rehabilitation guide or injury prevention exercise menu. The review is simply a list of variables to consider when problem-solving Achilles tendon injuries.
From Acute to Chronic Achilles Tendinopathy
Injuries to the Achilles tendon can range from small, nearly trivial overuse reactions from a session to a complete rupture following years of suffering. In between these two extremes are partial tears, chronic degeneration, and other complex pathologies. Without getting into strict terminology, Achilles injuries are either chronic or acute and sometimes a combination of both. Endurance athletes tend to suffer overuse syndromes due to repetitive use and general overload, and speed and power athletes are prone to tears from jumping and cutting rapidly.
Freak injuries occur that have ruined careers, for example an athlete slipping at home. These random injuries leave biomechanics experts and medical doctors perplexed. The reasons many athletes injure their Achilles, however, is not a mystery nor a big surprise. They have common risk factors and variables that either increase the likelihood of injury or overlap other injures.
I’m not qualified to diagnose a true injury unless I witness or hear the tear and see the gruesome disfigurement of the calf and ankle immediately afterward. If you look for a diagnosis over the internet, you’ll be very disappointed. If you want a list of symptoms and a way to gauge the severity of an injury, I recommend seeing a medical professional. Coaches are the first responders. And because sports medicine practitioners are only consulted when training is impaired, it’s important to work collaboratively with your organization’s medical staff or connect with a really good therapist.
The Usual Suspects for Achilles Tendon Injuries
Below is a list of risk factors, some well documented and a few slightly theoretical, that contribute to the occasional complex storm of variables that injure the tendon. Many are not unique to Achilles injuries, as general mistakes in training are often the issue, while others focus on compensation injuries to the tendon.
Previous Injury
Athletes with recent or past injuries to their tendon structure are at risk for Achilles tendon injuries. What’s disappointing is that many sport athletes have their injuries documented publically, leading to speculation of when, and not if, a more severe injury will follow. Seattle Seahawks cornerback Richard Sherman struggled for weeks with an Achilles problem before his rupture on live TV.
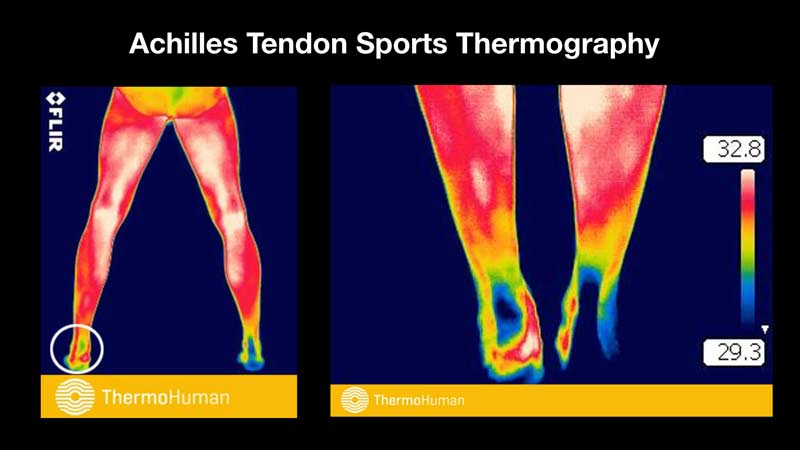
Direct Achilles injuries may not be the only previous injury that causes problems. Other soft tissue and joint injuries may predispose an athlete due to compensation. Record keeping and high-resolution medical imaging are excellent ways to ensure good management of past problems so they won’t resurface from neglect and oversite.
Athlete Genetics and Age
Older male athletes are more prone to injury. For those athletes who have less mileage on their body, age and genetics will conspire against most of them. Some promising genetic research may help identify why some athletes are more likely to get injured because they’re ill-equipped by their DNA. I’m not excited enough about this yet to invest in screening kits for my practice or to make financial investments in a company’s stock.
I do believe there’s a connection between injuries and genetics, but so far it’s very early, and most consumer products don’t help coaches. There’s a lot of good supporting research about alpha 1 type V collagen (COL5A1), but it’s not enough to make me believe we cannot address the issue with training and recovery. We could argue a case for genetics by looking at the Wilkins’ brothers in the NBA, as both tore Achilles tendons at roughly the same age. Except DNA isn’t the only contributor to tendon injuries.
Foot Mechanics and Anatomy
The foot’s structure and function are directly related to risks of tendinopathy. The relationship is so small and specific, however, that a clean table of cause and effect isn’t available. For example, a Haglund’s deformity, a structural issue that sometimes causes mechanical wear to the tendon and bursa, has conflicting data. Still, the range of foot types and how they function will influence how the tendon receives mechanical strain.
Foot types and how they function impact how tendons receive mechanical strain, says @spikesonly. Share on XOversimplified reductionist labels like flat feet and pronator don’t move the chains of progress with pathomechanics because we need high granularity to connect how foot mechanics and the Achilles tendon coordinate. While advanced foot modeling in the laboratory is promising, even elite athletes still struggle and often resort to homemade interventions by coaches and medical staff. While the body is a living organism and able to self-repair, limits to regeneration rates exist, causing a race between tissue rebuilding and the tissue degeneration caused by mechanical stress.
Sporting Technique
Running biomechanics and sport movement competency are difficult variables to prove or disprove. And though they may not have enough impact to identify in isolation with laboratory tests, they could be the straw that breaks the camel’s back with sport. Studies on heel strike, forefoot, and midfoot landings have examined various populations for years, but most don’t take into account other variables like the ones listed here. Some movements stress the Achilles more than others based on some primitive metrics, but how much is debatable.
From the findings presented at some conferences where additional dialogue was available, it seems we need clinical experience to fill the gap between rough research ideas and the precise issue for individual cases. Besides the specificity of foot landings of homogeneous mechanics during endurance running, specific strategies for team sports such as soccer are important. Athletes who jog with a gait that’s unhealthy for their tendons may be unable to change their mechanics. Motor skills, for example, are stubborn later in a career.
Sports Nutrition
An athlete’s diet won’t bulletproof a doomed athlete, but several studies are showing that nutrition can influence collagen repair. There’s always an issue with consistency, however, as some foods and nutrients will not show up in blood chemistry tests and other methods used to evaluate athlete compliance. A few recent interventions are providing a realistic hope, including the combination of vitamin C and gelatin, but putting a lot of weight on a few studies is dangerous. I usually find that diets focusing on one or two key ingredients for healing end up failing the athlete, who doesn’t get all the nutrients they need.
A healthy diet can reduce #biomarkers for inflammation levels, says @spikesonly. Share on XWe don’t know why some athletes have higher inflammation levels than others, but a good diet can reduce the biomarkers. Healthy eating beyond a few supplements is necessary to reduce total body inflammation, but we need more research.
Training Programs
Eccentric exercise and general strength and conditioning programs can theoretically help athletes with Achilles tendon problems, but nothing is perfect. Sometimes rest with immobilization or slight support can start the healing process better than training modifications. Heavy tension on the tendon at slower speeds while performing negative work to the tissues is successful in many studies. What is less researched is the general capacity to heal and regeneration of local areas from global programs similar to the effects of blood flow restriction training and uninjured limb training on specific injuries.

Some connections to weak posterior chain muscles, such as the glutes, are now available in limited research. But we find a chicken and egg scenario. Do weak glutes risk the tendons? Or does an Achilles tendon injury decrease recruitment of the glutes due to pain or changes to motion biomechanics? A competent and well-designed strength and conditioning program should reduce risk by preparing for the eccentric demands of intense training and competition.
Workload Management
Too much too soon, sudden changes in training, and other volume and intensity errors are common culprits for injuries. Not everyone suffers injuries when workloads are too high. Theoretically, a gradual training buildup should make an athlete more resilient. So far, however, no research supports the idea that, like bones, more stress will improve the tendon; degeneration commonly occurs in many athletes.
No research supports the idea that more workload stress will improve the tendons, says @spikesonly. Share on XProfessional sport teams tend to rest players to solve injuries, but so far that has not worked either. Being prepared for the rigors of a long season still require exposure to stimuli that create specific adaptations. Too much of the same stimuli can cause overuse syndromes—a reason cross-training became popular in the 1980s and 1990s.
Patterns of loading, such as the acute and chronic work ratio, have tried to mitigate injuries with controlled buildup and capacity, although this strategy has fallen short for many reasons. It’s fair to say that a reasonable management strategy can keep an athlete healthy, but so far there are no details strong enough for me to list or stand behind scientifically.
Surfaces and Terrain
Athletes are exposed to different surfaces during competition and practice venues with various limitations and randomness, or they live on the same surface all the time. NBA athletes live on the hardwood for months without access to soft options like grass. Track athletes can rotate surfaces. Endurance athletes have the most options, including hills and trails. Some terrain may create variety while others like sand are not valuable for athletes and actually may risk the Achilles tendon.

Many coaches have theorized that progressions from grass to track effectively build up the tendons, but so far this is hard to prove; the individualization required on surfaces is very specific and difficult to identify systemically. Some natural grass fields are useful for speed and power athletes, along with trails for endurance athletes, and are worth using during the general preparation phase.
Athletic Footwear
The controversy over spikes, sneakers, skates, and orthotics continues from year to year. Marketing hype from shoe companies and the poor validations by studies from some journals leaves those of us in the field asking the same questions every season. What is the right shoe for my athlete, and do athletes need orthotics? It will be a long time before studies sufficiently demonstrate that clinical evaluations of the foot and the changes made by shoes and orthotics have any true meaning.
What’s notable now is that big differences exist ranging from barefoot to shod options. Although the differences between shoes are very small, they may be enough to cause risk to pathology. An obvious example of extreme designs are the strength shoes from the early 1990s that clearly created problems. If training causes the issue in the first place, slight changes in heel drop, insole stiffness, and materials can help. Pressure mapping, motion capture, EMG, and medical imaging can create a good case for what matters and what is so trivial it’s not worth thinking about.
Medications and Drugs
The last factor is medications, both injectable drugs and over the counter medications. We’ve seen some antibiotic research on Achilles injuries using observational studies, but actual direct cause and effect aren’t clear. The FDA has stated that there’s a strong link between the two, but the research shows nothing groundbreaking explaining the reasons why, other than general physiological explanations.
Other medications have a slight connection. Corticosteroids injections sometimes receive blame due to location inaccuracy of manual injections. Corticosteroids also mask pain so athletes can push through a problem and experience poor remodeling. From the research, it’s clear that the Achilles tendon doesn’t respond well to drugs, so we must weigh many pharmacological interventions against legal conflicts (WADA) and contraindications to healing.
Other Risk Factors
I’m sure other risk factors exist, but I doubt any of them are important. As we see more research published, we’ll acquire more details to help us make changes or smarter choices to reduce risks further. Being aware of the above list and making efforts to address as many as possible within reason will give most of us the peace of mind to try to control the controllable.
When to See a Specialist
I recommend seeing a very thorough podiatrist, who uses radiology, for a second opinion. Progressive and knowledgeable podiatrists will do both a clinical evaluation and a gait analysis. A podiatrist who simply recommends orthotics from a glance at your feet and a very brief conversation about symptoms should be ignored. A lot of great physical therapists are available, but most of them are not specialists and don’t have enough training to master the complexities of the foot.
Consulting specialists who are experts in Achilles tendon problems, especially those who have experience working in sports, is priceless. Don’t wait for the problem to get out of control. Catching the injury early can save a dream from being destroyed.
Since you’re here…
…we have a small favor to ask. More people are reading SimpliFaster than ever, and each week we bring you compelling content from coaches, sport scientists, and physiotherapists who are devoted to building better athletes. Please take a moment to share the articles on social media, engage the authors with questions and comments below, and link to articles when appropriate if you have a blog or participate on forums of related topics. — SF
[mashshare]



